

BETA-THALASSEMIA TREATMENTS
Transplant
What happens during a stem cell transplant?
Stem cells are most often found in the bone marrow. Blood stem cells have the unique ability to grow and transform into other cells, like red blood cells and white blood cells. A stem cell transplant aims to replace blood stem cellsBlood stem cellan immature cell that has the potential to develop into all types of blood cells, including white blood cells, red blood cells, and platelets that contain a nonfunctioning HBB gene with blood stem cells from a donor who has a working HBB gene. A stem cell transplant from a donor adds healthy stem cells to the body.
Before the new cells are added, a form of treatment called conditioning (which is often chemotherapy) is used to make room in the bone marrow for new cells. Over time, the goal of a stem cell transplant is for the healthy blood stem cells to make their way to the bone marrow and start to make new blood cells; this process is known as engraftment.
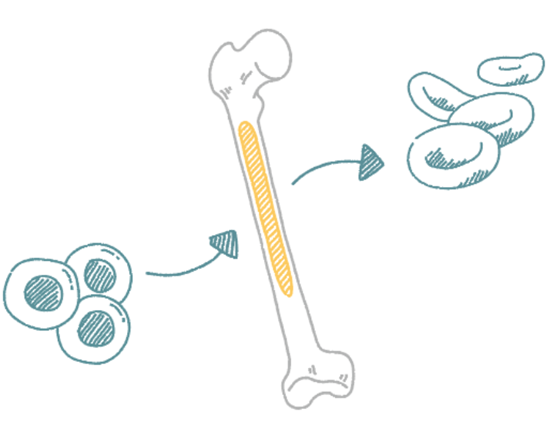
Stem Cell Transplants: What Should You Know?
Eligibility
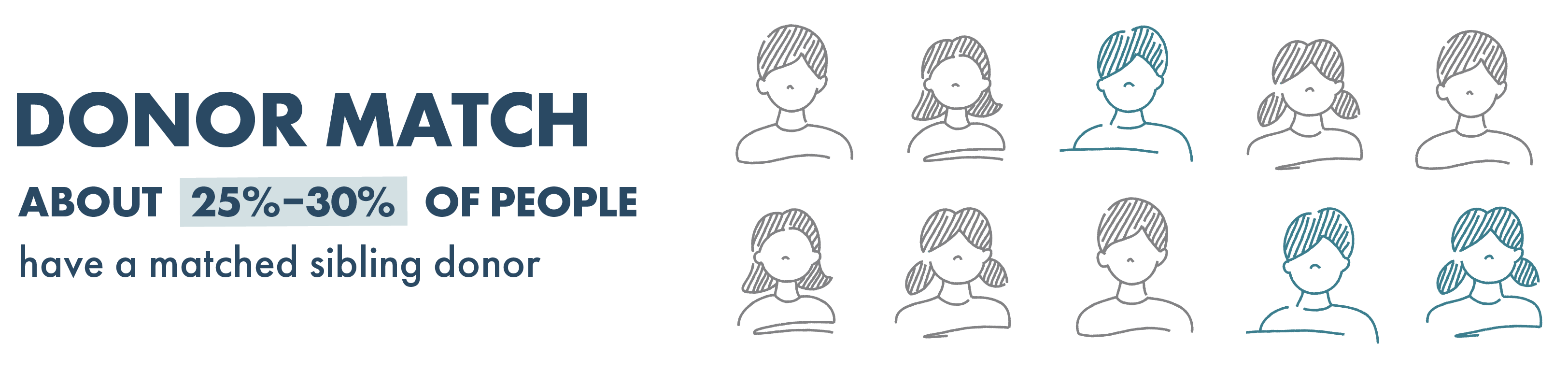
To receive a stem cell transplant, an appropriate stem cell donor (who may be related or unrelated to the patient) must be identified. This gives the transplanted cells the best chance of being accepted by your body. For the most favorable outcome, the donor should be genetically similar to the person receiving the stem cells, with the receiver being less than 14 years old. Generally, siblings are the people who are most genetically similar. Only about 25% to 30% of people have a matched sibling donor.
LIKELINESS OF A MATCHED SIBLING DONOR

If you want to learn more about this treatment option, it’s important to talk to your doctor about the benefits and potentially severe risks involved with stem cell transplants.
Complications
Although stem cell transplants have the potential to cure beta-thalassemia, there are also serious risks associated with this type of transplant. One major complication is a condition called graft-versus-host disease (GvHD). In GvHD, the transplanted stem cells see the body's cells as foreign, and thus attack them. GvHD severity can vary, but for some it can be a potentially serious complication, and even life-threatening in some cases.
 This website is developed by bluebird bio, Inc. and is intended for residents of the United States who are 18 years and older.
This website is developed by bluebird bio, Inc. and is intended for residents of the United States who are 18 years and older.